| Acute Bronchitis (bron-KITE-is) is swelling and irritation of the windpipe (trachea) or the airways to the lungs. It occurs most often in the winter and usually starts as a cold. The cold then spreads from the nose and throat to the windpipe and airways. 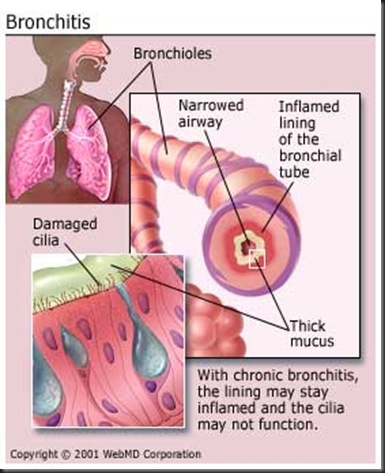
Causes This disease is usually caused by germs (virus or bacteria) spread through the air or by contact with someone who is infected. Other causes are allergies or breathing air that contains chemical fumes, dust, or smoke. Your chances of getting bronchitis increase if you have lung disease, smoke, go out in cold, humid weather, do not eat healthy foods, or have become run down from another illness. Signs/Symptoms The most common symptom is a dry cough. Later in the illness the cough may bring up sputum. Other complaints may include a low fever (less than 101 degrees F (38.3 degrees C), burning chest pain or pressure behind the breastbone, noisy breathing (wheezing), and trouble breathing. Care Most people can be treated at home. Care may include cough medicine to control the cough (suppressants) and cough expectorants to thin the sputum. Antibiotics may also be needed to fight an infection caused by bacteria. You may need to be put into the hospital if you get pneumonia or chronic bronchitis, or if you fail to get better. Risks If you don't follow your doctor's directions, your illness can get worse or turn into pneumonia. Remember, acute bronchitis can be cured with medicine. WHAT YOU SHOULD DO - Always take your medicine as directed. If you feel it is not helping, call your doctor. Do not quit taking it on your own.
- If you are taking antibiotics, continue to take them until they are all gone even if you feel well.
- If you are taking medicine that makes you drowsy, do not drive or use heavy equipment.
- If you use medicine that you inhale, follow the steps below:
- First, shake the inhaler.
- Breathe out slowly, all the way.
- Put the mouthpiece of the inhaler in your mouth or 2 inches away (about half a finger's length), or use the spacer (a piece of plastic-like tubing that attaches to the inhaler).
- Breathe in and push down on the inhaler at the same time (to create the mist).
- Hold your breath for about 10 seconds.
- Breathe out slowly through puckered lips or through your nose.
- If you need to take 2 puffs, wait 2 to 5 seconds before taking the second one.
- Gargling after using your inhaler may reduce burning in your throat.
- Quit smoking. It increases your chances of getting lung diseases such as bronchitis, and harms the heart and lungs. If you are having trouble quitting, ask your doctor for help.
- If you are coughing up sputum and milk seems to make your sputum thicker, avoid dairy foods.
- If you do not have to limit the amount of liquids you drink, drink 8 to 10 (soda-can sized) glasses of water each day. This helps thin the sputum so it can be coughed up more easily.
- To help keep your lungs free of infection, take 2 or 3 deep breaths and then cough. Do this often during the day.
- Use a humidifier to help keep the air moist and your sputum thin. This makes it easier to cough up the sputum. You must keep the humidifier free of fungus. Clean it every day.
- Stay inside during very cold or hot weather, or on days when the air pollution is high. This will help you breathe easier and help control your cough.
- Rest until you feel better. You may return to work or school when your temperature is around 98.6 degrees F (37 degrees C).
Call Your Doctor If... - Your cough does not go away in a few days.
- You have a rash, itching, swelling, or stomach pain or any other problems that might be caused by your medicine.
- You cough up gray, green, or bloody sputum.
Seek Care Immediately If... - You have chills, increasing chest pain, trouble breathing while resting, or vomiting.
- Your lips or nailbeds turn blue or pale.
- You are coughing and cannot stop, or your constant coughing makes you feel light-headed.
IF YOU'RE HEADING FOR THE HOSPITAL... What to Expect While You're There You may encounter the following procedures and equipment during your stay. - Activity: At first you will need to rest in bed, with a few pillows to keep you sitting up a little. This will help your breathing. Do not lie flat. Once you are breathing more easily, you will be allowed to increase your exercise.
- Oxygen: You may need extra oxygen at this time. It is given either by a mask or nasal prongs. Tell your doctor if the oxygen is drying out your nose or if the nasal prongs bother you.
- Pulse Oximeter: While you are getting oxygen, you may be hooked up to a pulse oximeter (ox-IM-uh-ter). It is placed on your ear, finger, or toe and is connected to a machine. It measures the oxygen in your blood.
- IV: A tube placed in your vein for giving medicine or liquids. It will be capped or have tubing connected to it.
- Medicines: The drugs below will help you breathe easier. They can be taken by mouth or given in your IV.
- Antibiotics: If you have an infection in the lungs, you'll be given antibiotics to clear it up.
- Bronchodilators (bronk-o-DIE-lay-tors): The medicines may be needed to help open your lung's airways.
- Steroids (STAIR-oids): You may be given one of these drugs to decrease the swelling and inflammation of the tissue in your lungs.
- Breathing Treatments: A machine will be used to help you inhale medicine. A therapist will help with these treatments. They will help open your airways so you can breathe easier. At first you may need them frequently. As you get better, you may only need them when you are having trouble breathing.
- Postural Drainage: A nurse may tap your back briskly with his or her hands. This helps loosen the sputum in your lungs so you can cough it up more easily.
- Taking Vital Signs: These include your temperature, blood pressure, pulse (counting your heartbeats), and respirations (counting your breaths). A stethoscope is used to listen to your heart and lungs. Your blood pressure is taken by wrapping a cuff around your arm.
- ECG: Also called a heart monitor, an electrocardiograph (e-lec-tro-CAR-dee-o-graf), or EKG. The patches on your chest are hooked up to a TV-type screen or a small portable box (telemetry unit). This screen shows a tracing of each heartbeat. Your heart will be watched for signs of injury or damage.
- 12 Lead ECG: This test makes tracings from different parts of your heart. It can help your doctor decide whether there is a heart abnormality.
- Chest X-ray: This picture of your lungs and heart will be used to monitor your condition.
- Blood Gases: Blood taken from an artery in your wrist, elbow, or groin is tested for oxygen.
- Blood: Usually taken for testing from a vein in your hand or from the bend in your elbow.
|

No comments:
Post a Comment