Diseases of the heart valves are grouped according to which valve or valves are involved and the amount of blood flow that is disrupted by the problem. The most common and serious valve problems happen in the mitral and aortic valves. Diseases of the tricuspid and pulmonary valves are fairly rare.
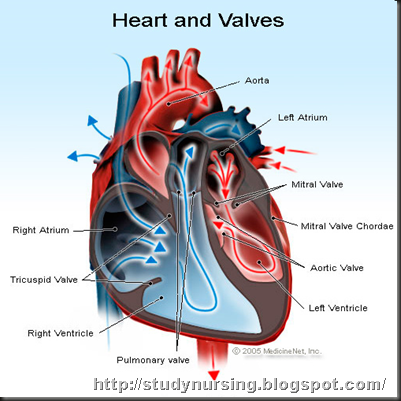 The mitral valve regulates the flow of blood from the upper-left chamber (the left atrium) to the lower-left chamber (the left ventricle).
The mitral valve regulates the flow of blood from the upper-left chamber (the left atrium) to the lower-left chamber (the left ventricle).
Here we will discuss 3 diseases of the mitral valve: mitral valve prolapse, mitral regurgitation, and mitral stenosis.
Mitral valve prolapse
Mitral valve prolapse (also known as "click murmur syndrome" and "Barlow's syndrome") is the most common heart valve abnormality, affecting five to ten percent of the world population. A normal mitral valve consists of two thin leaflets, located between the left atrium and the left ventricle of the heart. Mitral valve leaflets, shaped like parachutes, are attached to the inner wall of the left ventricle by a series of strings called "chordae." When the ventricles contract, the mitral valve leaflets close snugly and prevent the backflow of blood from the left ventricle into the left atrium. When the ventricles relax, the valves open to allow oxygenated blood from the lungs to fill the left ventricle.
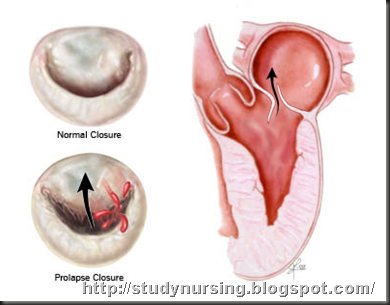 In patients with mitral valve prolapse, the mitral apparatus (valve leaflets and chordae) becomes affected by a process called myxomatous degeneration. In myxomatous degeneration, the structural protein collagen forms abnormally and causes thickening, enlargement, and redundancy of the leaflets and chordae. When the ventricles contract, the redundant leaflets prolapse (flop backwards) into the left atrium, sometimes allowing leakage of blood through the valve opening (mitral regurgitation). When severe, mitral regurgitation can lead to heart failure and abnormal heart rhythms. Most patients are totally unaware of the prolapsing of the mitral valve. Others may experience a number of symptoms discussed below.
In patients with mitral valve prolapse, the mitral apparatus (valve leaflets and chordae) becomes affected by a process called myxomatous degeneration. In myxomatous degeneration, the structural protein collagen forms abnormally and causes thickening, enlargement, and redundancy of the leaflets and chordae. When the ventricles contract, the redundant leaflets prolapse (flop backwards) into the left atrium, sometimes allowing leakage of blood through the valve opening (mitral regurgitation). When severe, mitral regurgitation can lead to heart failure and abnormal heart rhythms. Most patients are totally unaware of the prolapsing of the mitral valve. Others may experience a number of symptoms discussed below.
The mitral valve prolapse (MVP) syndrome has a strong hereditary tendency, although the exact cause is unknown. Affected family members are often tall, thin, with long arms and fingers, and straight backs. It is seen most commonly in women from 20 to 40 years old, but also occurs in men.
What are the signs and symptoms of mitral valve prolapse?
Most people with mitral valve prolapse have no symptoms, however, those who do commonly complain of symptoms such as fatigue, palpitations, chest pain, anxiety, and migraine headaches. Stroke is a very rare complication of mitral valve prolapse.
Fatigue is the most common complaint, although the reason for fatigue is not understood. Patients with mitral valve prolapse may have imbalances in their autonomic nervous system, which regulates heart rate and breathing. Such imbalances may cause inadequate blood oxygen delivery to the working muscles during exercise, thereby causing fatigue.
Palpitations are sensations of fast or irregular heart beats. In most patients with mitral valve prolapse, palpitations are harmless. In very rare cases, potentially serious heart rhythm abnormalities may underlie palpitations which require further evaluation and treatment.
Sharp chest pains are reported in some patients with mitral valve prolapse, which can be prolonged. Unlike angina, chest pain with mitral valve prolapse rarely occurs during or after exercise, and may not respond to nitroglycerin.
Anxiety, panic attacks, and depression may be associated with mitral valve prolapse. Like fatigue, these symptoms are believed to be related to imbalances of the autonomic nervous system.
Migraine headaches have been occasionally linked to mitral valve prolapse. They are probably related to abnormal nervous system control of the tension in the blood vessels in the brain.
Mitral valve prolapse may be rarely associated with strokes occurring in young patients. These patients appear to have increased blood clotting tendencies due to abnormally sticky blood clotting elements, called platelets.
How is mitral valve prolapse diagnosed and evaluated?
Examination of the patient reveals characteristic findings unique to mitral valve prolapse. Using a stethoscope, a clicking sound is heard soon after the ventricle begins to contract. This clicking is felt to reflect tightening of the abnormal valve leaflets against the pressure load of the left ventricle. If there is associated leakage (regurgitation) of blood through the abnormal valve opening, a "whooshing" sound (murmur) can be heard immediately following the clicking sound.
Echocardiography (ultrasound imaging of the heart) is the most useful test for mitral valve prolapse. Echocardiography can measure the severity of prolapse and the degree of mitral regurgitation. It can also detect areas of infection on the abnormal valves. Valve infection is called endocarditis and is a very rare, but potentially serious complication of mitral valve prolapse. Echocardiography can also evaluate the effect of prolapse and regurgitation on the functioning of the muscles of the ventricles.
Abnormally rapid or irregular heart rhythms can occur in patients with mitral valve prolapse, causing palpitations. A 24-hour Holter monitor is a continuous cassette recording of the patient's heart rhythm as the patient carries on his/her daily activities. Abnormal rhythms occurring during the test period are captured on tape and analyzed at a later date. If abnormal rhythms do not occur every day, the Holter recording may fail to capture the abnormal rhythms. These patients then can be fitted with a small "event-recorder" to be worn for up to several weeks. When the patient senses a palpitation, an event button can be pressed to record the heart rhythm prior to, during, and after the palpitations.
What is the treatment for mitral valve prolapse?
The vast majority of patients with mitral valve prolapse have an excellent prognosis and need no treatment. For these individuals, routine examinations including echocardiograms every few years may suffice. Mitral regurgitation in patients with mitral valve prolapse can lead to heart failure, heart enlargement, and abnormal rhythms. Therefore, mitral valve prolapse patients with mitral regurgitation are often evaluated annually. Since valve infection, endocarditis, is a rare, but potentially serious complication of mitral valve prolapse, patients with mitral valve prolapse are usually given antibiotics prior to any procedure which can introduce bacteria into the bloodstream. These procedures include routine dental work, minor surgery, and procedures that can traumatize body tissues such as colonoscopy, gynecologic, or urologic examinations. Examples of antibiotics used include oral amoxicillin and erythromycin as well as intramuscular or intravenous ampicillin, gentamycin, and vancomycin.
Patients with severe prolapse, abnormal heart rhythms, fainting spells, significant palpitations, chest pain, and anxiety attacks may need treatment. Beta-blockers, such as atenolol (Tenormin), metoprolol (Lopressor), and propranolol (Inderal), are the drugs of choice. These act by increasing the size of the left ventricle, thereby reducing the degree of prolapse. The calcium blockers verapamil (Calan) and diltiazem (Cardizem) are useful in patients who cannot tolerate beta-blockers.
Although most patients with mitral valve prolapse require no treatment or treatment with oral medications, in very rare cases, surgery (mitral valve replacement or repair) may be required. Patients who require surgery usually have severe mitral regurgitation causing worsening heart failure and progressive heart enlargement. Rarely, rupture of one or more chordae can cause sudden, severe mitral regurgitation and heart failure requiring surgical repair. Mitral valve repair is preferable if possible, to mitral valve replacement as the surgical treatment for mitral valve regurgitation. After mitral valve replacement, lifelong blood thinning medications are necessary to prevent blood from clotting on the artificial valves. After mitral valve repair, these blood thinning medications are unnecessary. Because of the success of valve repair, it is being performed earlier in patients with mitral regurgitation, thus reducing the risk of abnormal heart rhythms and heart failure.
Rare patients with mitral valve prolapse may suffer strokes because of increased blood clotting. These patients can be treated with a combination of a blood thinner (anticoagulant) and a beta-blocker.
Again, although patients with mitral valve prolapse may experience a variety of complications, most have no symptoms and can lead healthy, active, and normal lives.
Mitral Valve Prolapse At A Glance
- Mitral valve prolapse (mitral valve prolapse) is the most common heart valve abnormality.
- Most patients with mitral valve prolapse have no symptoms and require no treatment.
- Mitral valve prolapse can be associated with fatigue and/or palpitations.
- Mitral valve prolapse can often be detected by a doctor during examination of the heart. mitral valve prolapse can be confirmed with an echocardiogram.
- Patients with mitral valve prolapse are usually given antibiotics prior to any procedure which might introduce bacteria into the bloodstream, including dental work and minor surgery.
Mitral Regurgitation
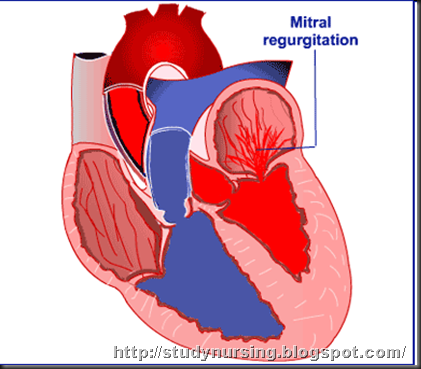
Mitral regurgitation is also called mitral insufficiency or mitral incompetence. It happens when the mitral valve allows a backflow of blood into the heart's upper-left chamber (the left atrium). Mitral regurgitation may take years to reveal itself. But, if it goes on long enough, it can cause a buildup of pressure in the lungs or cause the heart to enlarge. In time, this will lead to symptoms.
 What causes mitral regurgitation?
What causes mitral regurgitation?
Mitral regurgitation is usually caused by conditions that weaken or damage the valve. The most common causes of mitral regurgitation in adults are listed below.
- Valve damage from rheumatic fever during childhood.
- Injury to the mitral valve after a heart attack.
- Injury to the mitral valve from an infection of the heart's inner lining (called infective endocarditis).
What are the symptoms?
In most cases, symptoms come on slowly. They may include
- Heart palpitations (the feeling that the heart has skipped a beat).
- Shortness of breath.
- Fast breathing.
- Chest pain.
- Coughing.
- Fatigue.
If you have mitral regurgitation, you should talk to your doctor about taking antibiotic medicine before dental procedures or general surgery. The medicine will prevent infection of the valve. Mitral regurgitation may also lead to heart failure, stroke, irregular heartbeat (arrhythmia), and blood clots in the lungs (pulmonary emboli).
Mitral Stenosis
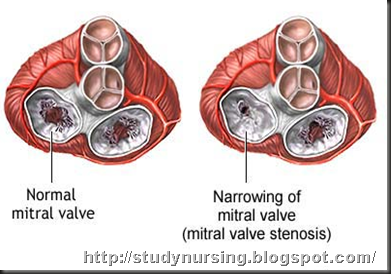
Mitral stenosis is a narrowing or blockage of the mitral valve. The narrowed valve causes blood to backup in the heart's upper-left chamber (the left atrium) instead of flowing into the lower-left chamber (the left ventricle). Most adults with mitral stenosis usually had an infection called rheumatic fever when they were younger. Mitral stenosis may also be associated with aging and a buildup of calcium on the ring around the valve where the leaflet and heart muscle meet. Cases of mitral stenosis are fewer in developed countries because of the medicines used to fight the infections that lead to rheumatic fever.
Mitral stenosis is usually caused by rheumatic fever, but it can be caused by any condition that causes narrowing of the mitral valve. The condition is rarely passed down through family members.
What are the symptoms?
Most people with mitral stenosis have no symptoms. When symptoms do happen, they may get worse with exercise or any activity that increases your heart rate. These may include
- Trouble breathing at night or after exercise.
- Coughing, which sometimes produces a pinkish, blood-tinged sputum.
- Fatigue.
- Chest pain that gets worse with activity and goes away with rest.
- Frequent respiratory infections such as bronchitis.
- Heart palpitations (the feeling that the heart has skipped a beat).
- Swelling (edema) of the feet and ankles.
- A hoarse or husky-sounding voice.
Symptoms may begin with an episode of atrial fibrillation. Pregnancy, a respiratory infection, endocarditis, or other cardiac conditions may also cause symptoms. Mitral stenosis may eventually lead to heart failure, stroke, or blood clots to various parts of the body.
No comments:
Post a Comment