A gastrojejunostomy is the surgical creation of an opening in the stomach to connect it to the upper portion of the small bowel, or small intestine, so that the surgeon can place a tube into the opening. The tube allows medications and nutritional liquids to be given through the tube directly into the stomach.
Indication
Gastrojejunostomies are performed on patients who cannot eat normally or take medicine orally due to a blockage or cancer of the stomach or pancreas. Some patients who have a condition that causes an obstructed bowel may undergo a gastrojejunostomy if they are unable to have a nasogastric tube, a tube that runs from the nose into the stomach.
Description
This procedure is typically performed with surgery, where an incision is made in the stomach. Precutaneous gastrojejunostomies are performed through a very small incision, much smaller than that usually required for a normal gastrojejunostomy. Interventional radiologists perform precutaneous gastrojejunostomies, and these procedures usually result in fewer complications and quicker recovery times.
Procedure
Patients preparing for a gastrojejunostomy should not eat or drink for at least six hours prior to surgery so that there is no fresh food or liquid in the stomach. Patients should advise their doctors and surgeons of any medications they are currently taking prior to surgery. Some medications, such as blood thinners, may need to be reduced or stopped several weeks prior to surgery to minimize the risk of excessive bleeding and other potential complications. Patients should also advise their doctors of any allergies, previous reactions to anesthesia, and any chronic health conditions.
Gastrojejunostomies are performed under general anesthesia, usually given intravenously through an IV line. Precutaneous gastrojejunostomy procedures are usually done with a local anesthetic and sleeping medication. Patients who have precutaneous gastrojejunostomies still require an IV line so that the surgeon can administer fluids, painkillers, antibiotics, and other medications as necessary.
An ultrasound is usually used to help the surgeon or interventional radiologist determine where to place the gastrojejunostomy tube. The tube is usually placed right before the rib cage. The patient's stomach is inflated with air through a tube that runs through the nose into the stomach so that the surgeon can place the tube properly.
Precutaneous gastrojejunostomies involve the stomach being fastened to the inside of the abdomen with small clips that are inserted through the skin. The clips are removed once the procedure is complete.
Procedure: Laparoscopic Gastrojejunostomy (stomach-small bowel connection)
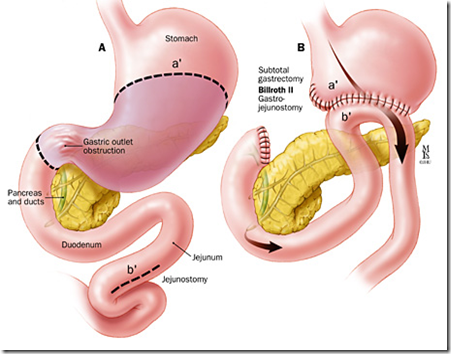
A. The Condition. You may have a condition in which food cannot pass out of your stomach. In this situation, your surgeon will bypass the blockage by connecting your intestine directly to your stomach. Dr. Frantzides was the first in the world to perform and publish a laparoscopic gastroduodenostomy for gastric outlet obstruction in 1996.
B. Symptoms
- Nausea, vomiting
- Crampy abdominal pain
- Weight loss, weakness
C. Laparoscopic Gastrojejunostomy.
The surgeon will make about 3-4 small incisions in your abdomen. A port (nozzle) is inserted into one of the slits, and carbon dioxide gas inflates the abdomen. This process allows the surgeon to see inside of your abdomen more easily. A laparoscope is inserted through another port. The laparoscope looks like a telescope with a light and camera on the end so the surgeon can see inside the abdomen. Surgical instruments are placed in the other small openings and used to connect the small intestine (jejunum) to the stomach. This is done with surgical staplers. After this has been accomplished, the carbon dioxide is released out of the abdomen through the slits, and then these sites are closed with sutures or staples, or covered with glue-like bandage and steri-strips.
D. Nonsurgical Treatment.
Sometimes your problem may be treated with suctioning out the stomach, withholding food for several days, and giving IV fluids. Your doctor will discuss with you what your best option is.
E. Risks. The primary risks of laparoscopic gastrojejunostomy are:
- Infection of the skin at one of the small ports sites
- Leakage of the connection between the stomach and small bowel
- Collection of pus inside your abdomen (intraabdominal abscess)
- Postoperative ileus (the intestines slow down/stop working for several days)
- Small bowel obstruction (kinking of the small bowel, causing blockage)
F. Expectations
1. Before Your Operation. Laparoscopic gastrojejunostomy usually is an elective procedure. The preoperative evaluation might include blood work, urinalysis, a barium swallow x-ray, endoscopy (looking down your throat with a scope), and perhaps an abdominal CT scan. If you smoke, then you should stop immediately. If you are taking blood thinners (for example, aspirin, coumadin, Lovenox, or Plavix), then you will need to stop these one week prior to your procedure. Your surgeon and anesthesia provider will review your health history, medications (including blood thinners), and options for pain control.
2. Your Recovery. You usually can go home in 2-4 days after a laparoscopic gastrojejunostomy. You may need to wait until your bowels start working. You will be given medication for pain. You should limit your activity to light lifting (no more than 15 lb) for one month.
3. Inform Surgeon if you have one or more of the following:
- High fever
- Severe abdominal pain
- Odor or increased drainage from your incision
- No bowel movements for three days
Nursing considerations
Client Assessment Database
Data depend on the underlying condition necessitating surgery.
Teaching/Learning
Discharge plan
considerations: Assistance with administration of enteral feedings/total parenteral nutrition (TPN) if required, and acquisition of supplies
Refer to section at end of plan for postdischarge considerations.
Nursing Priorities
1. Promote healing and adequate nutritional intake.
2. Prevent complications.
3. Provide information about surgical procedure/prognosis, treatment needs, and concerns.
Discharge Goals
1. Nutritional intake adequate for individual needs.
2. Complications prevented/minimized.
3. Surgical procedure/prognosis, therapeutic regimen, and long-term needs understood.
4. Plan in place to meet needs after discharge.
- 1. NURSING DIAGNOSIS: risk for imbalanced Nutrition: less than body requirements
- 2. NURSING DIAGNOSIS: deficient Knowledge [Learning Need] regarding
- procedure, prognosis, treatment, self-care, and discharge needs
POTENTIAL CONSIDERATIONS following acute hospitalization (dependent on client’s age, physical condition/presence of complications, personal resources, and life responsibilities)
risk for Imbalanced Nutrition—less than body requirements—change in digestive process/absorption of nutrients, early satiety, gastric irritation.
Fatigue—decreased energy production, states of discomfort, increased energy requirements to perform activities of daily living (ADLs).
No comments:
Post a Comment